A Brighter Smile,
A Brighter Experience
Individualized dental care, personalized
treatment: awake, asleep, or at home
Bay Area Location
New York Location
Email Us
Emergency (24/7)
Emergency, In-Home, Sedation & General Dentistry
A Unique Dental Practice for Unique Patients
At the Blende Dental Group, we’re making it personal – a personalized approach to dental care, that is.
We are a unique medical-dental group with over 40 years of experience, some of the nation’s most specialized dentists, and a pioneering range of services that very few dental providers can offer, such as sedation or sleep dentistry, hospital dentistry, concierge dentistry, and house call dentistry for in-home care through advances in mobile dentistry. Our team is also on-call every day, including after hours and on weekends, to offer a same-day response to dental emergencies.
Our mission is to remove the barriers for receiving dental care through individualized treatment options: Awake (general patients), Asleep (sedation dentistry), or At Home (disabled, special needs, and homebound patients).
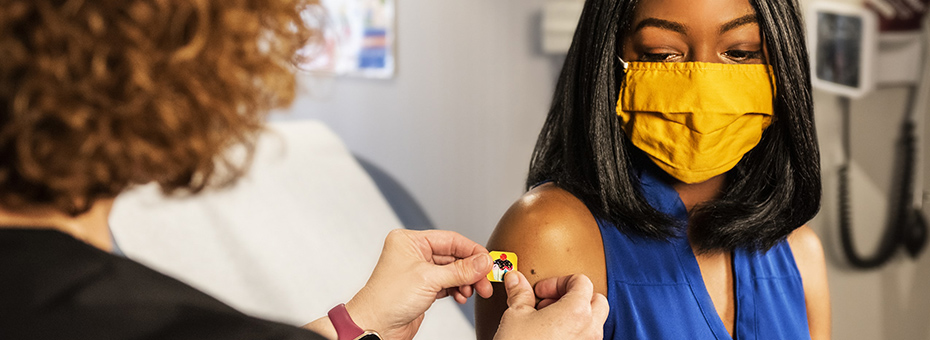
Awake
For all general dental needs, with treatment provided in our welcoming and disabled-accessible offices. Patients enjoy safe, long-lasting, and aesthetically pleasing results with predictable outcomes in the comfort of our San Francisco and New York City dental offices.
Asleep
Is receiving traditional dental care impossible because of phobias or physical, medical, or cognitive challenges? Sedation dentistry can help. Our team of medical dentists specializes in sedation options for those with complex needs. We are national leaders in sedation dentistry.
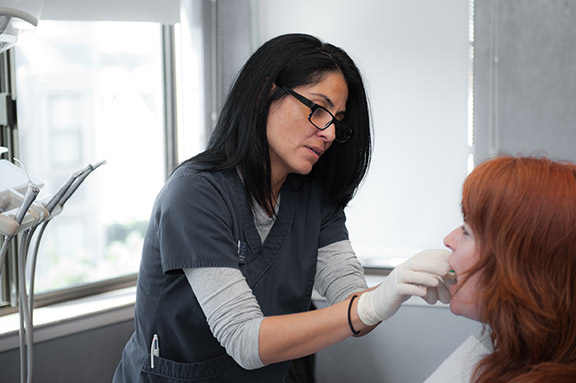
At Home
Are you or a loved one homebound? Let our dentists and hygienists come to you. We perform dental house calls through advanced mobile dentistry. We’re a national leader in treating seniors and people with special needs who can’t travel.
Who We Treat
The philosophy behind Awake, Asleep, and At Home dentistry comes from our staunch belief that dentistry should be available to any patient. Let us put a smile on your face while removing any barriers you or your loved ones have encountered when trying to access necessary care.
General Patients
From regular oral hygiene to concierge dentistry, Blende Dental Group offers the most comprehensive care. We provide routine dental cleanings, restorations, premier cosmetic dentistry, and enhanced care for complex cases—in our comfortable office locations.
Special Needs Patients
The Blende Dental Group has earned its reputation as a national leader in the treatment of patients with special needs by safely and successfully completing thousands of complex cases. We understand your needs and can help. For patients who have neglected dental visits due to phobias or special needs, we offer sedation, sleep, and hospital dentistry options from some of the country’s most respected dentists and specialists.
Seniors & Homebound Patients
Our House Call Dentists and hygienists deliver care in the safety of our patients’ homes when special needs, disabilities, or mobility issues make travel challenging or impossible.
Testimonials
Some Kind Words
Bill
Elizabeth
Shein
Arnette Davis
CPMC Nurse and General Patient
Taiko Hashimoto
Daughter of Emergency Patient who has dementia
Bill
Elizabeth
Shein
Arnette Davis
CPMC Nurse and General Patient
Taiko Hashimoto
Daughter of Emergency Patient who has dementia
Bill
Contact Us
San Francisco
Call The Office
Email Us
Office Location
390 Laurel Street
Suite 310
San Francisco, CA 94118
New York
Call The Office
Email Us
Office Location
150 East 58th St.
8th Floor Annex
New York, NY 10155
Our Latest Articles
Dental Health
It’s National Seafood Month, Time to Explore the Oral Health Benefits of Seafood for Those Pearly Whites
This National Seafood Month, explore the incredible oral health benefits of seafood and how it can transform your smile. October is National Seafood Month, a time to celebrate the bountiful…
bbadminist011
Dental Health
Mental Health Issues Affect Oral Health, But Specialized Dental Care Is Available
Each year, millions of Americans face the reality of living with mental health issues, but because of persistent stigmas and the fear of discussing these conditions, too few people seek…
bbadminist011
Dental Health
The Future of Dentistry: Embracing Innovation and Personalization
The future of dentistry is defined by innovation in techniques and technologies, with an emphasis on personalization and comfort. For those concerned about their oral health, a brighter future and…
bbadminist011
Oral Hygiene
October Is National Dental Hygiene Month – Tips and Tricks for Treating Yourself to a Cleaner Mouth
In 2009, the American Dental Hygienists’ Association (ADHA) helped launch National Dental Hygiene Month, which has been recognized annually in October since its inception. ADHA took these steps because it…
bbadminist011
All Posts
No White After Labor Day Shouldn’t Apply to Your Teeth: Here Are Some Tips for a Stunning Smile All Year
Outdated though the traditional may be, you could still face criticism from fashionistas for wearing white after Labor Day, a faux pas that invokes a throwback to the turn of…
bbadminist011
News
Happy Holidays from the Blende Dental Group
The end of any year is always a time of reflection. And when we look back on 2022, despite the challenges it presented around the world, we can't help but…
bbadminist011
Dental Health
How Dentistry Has Changed to Support Patients in the New Normal of Digital, On Demand, Concierge Care
According to research from the Federal Reserve Bank of New York, Americans got back 60 million hours of their time as a result of remote work during the pandemic. So…
bbadminist011
All Posts
Happy Thanksgiving from the Blende Dental Group
Thanksgiving is tomorrow, and as we write this, families across the nation are preparing to gather in a celebration of the bonds that unite us. The spirit of this season…
bbadminist011
All Posts
You May Be Surprised to Learn that Dental House Calls Not Only Exist, They’re Thriving
House calls are firmly ingrained in the fabric of American culture and history. We’ve all heard stories about the country doctor who traveled across hill and dale to care for…
bbadminist011
All Posts
No Tricks, Just Tips for a Healthy Mouth this Halloween
With Halloween falling on a Monday this year, weekend gatherings and All Hallows Eve trick-or-treating mean costumed revelers may have three days’ worth of sweets and goodies to enjoy. That’s…
bbadminist011
All Posts
Virtual Reality Could Become a Real World Benefit to Dentists and Their Patients
With leaps in the development of Virtual Reality (VR), could dentistry become part of Mark Zuckerberg’s metaverse? VR is being used as an educational tool for students and as an…
bbadminist011
All Posts
Blende Dental Group Thrilled to Participate in the International Association for Disability and Oral Health Conference in Paris
From August 23 to 26, the 26th conference of the International Association for Disability and Oral Health (iADH) takes place in Paris. “The rights of vulnerable populations to achieve an…
bbadminist011
All Posts
Cigarettes, Vapes and Marijuana, Oh My: The Oral Health Risks of Smoking
The good news? Tobacco use has reached an historic low. The bad news? Vaping (using electronic cigarettes filled with juice or nicotine salt) and marijuana use are climbing. Vaping may…
bbadminist011
All Posts
The Cosmetic Dentistry Market Is Booming, Thanks to Technology and Technique
According to the July report “Cosmetic Dentistry Market Size, Share, Trends, By Product Type, By Patient Type, By End-Use, and By Region Forecast to 2028,” cosmetic dentistry is booming. Analysts…
bbadminist011
All Posts
People with Special Needs Are Facing a Growing But Seldom Discussed Oral Health Crisis
It requires little effort to peruse the daily news and uncover stories related to the growing health crisis in the country, whether the issues involve post-pandemic outbreaks, staffing shortages for…
bbadminist011
All Posts
How Artificial Intelligence Will Shape the Future Reality of Dentistry
Artificial Intelligence (AI) and Augmented Intelligence (AuI), once inhabitants of a realm relegated to science fiction, have become increasingly ubiquitous aspects of modern life. Every day, people tap into the…
bbadminist011
All Posts
Bad Brushing Habits: Elbow Grease and Antiseptic Mouthwash Aren’t the Answer to Healthy Teeth
There’s an old joke that goes, “You brush your teeth at night to keep your teeth, you brush your teeth in the morning to keep your friends.” Humor aside, the…
bbadminist011
All Posts
Proudly Display a Healthier Smile this LGBTQ+ Pride Month
June 1 marks the first day of LGBTQ+ Pride Month. Equality, inclusion, acceptance, and support for friends and loved ones in the community are critical to the advancement of our…
bbadminist011
All Posts
Over-the-Counter or Professional Teeth Whitening? For the Brightest Smile, See Your Dentist
Memorial Day is right around the corner, signaling the start of summer. It’s also the season when people return to wearing white. However, the quest for a brighter, whiter smile…
bbadminist011
All Posts
You May Be Surprised at How Your Dentist Can Help with Sleep Apnea
May is a month of many health awareness events, including sleep. Created by the Better Sleep Council (BSC), Better Sleep Month seeks to raise awareness about the benefits associated with…
bbadminist011
All Posts
Before Ordering Another Round, Know How Alcohol Affects Oral Health
Need a drink after a rough day? Is it “beer-thirty” yet? Are you meeting colleagues for an adult beverage at the local happy hour? Have you been to Napa and…
bbadminist011
All Posts
Asthma, Allergies, and Dental Problems: What You Need to Know
In 1984, the Asthma and Allergy Foundation of America (AAFA) declared the month of May to be “National Asthma and Allergy Awareness Month.” They chose this time of year because…
bbadminist011
All Posts
Yes, Kissing Can Cause Cavities, So Plan a Date with Your Dentist Before Your Tinder Match
All the kids are on TikTok, they say. TikTok has emerged as an immensely popular social network that relies on short-form user videos that span genres such as pranks, stunts,…
bbadminist011
All Posts
Braces or Clear Aligners? The Choice Involves More than Appearance
For many teens and adults, orthodontics offers a clear path toward straighter teeth and a more confident smile. Misaligned teeth are common and don’t generally pose oral health risks. So…
bbadminist011
All Posts
Everyone’s Stressed Out, and It’s a Real Pain in the…Mouth
We learned a lot during the past two years of dealing with a pandemic. For many people, one of those things was the word “bruxism.” Dentists around the country have…
bbadminist011
All Posts
It’s Time to See the Dentist and Overcome the Pandemic’s “Dental Disaster”
Health officials are warning of fresh COVID-19 outbreaks with new variants such as BA.2.12 and BA.2.12.1, surging across the United States. The fallout from the pandemic’s initial outbreak severely impacted…
bbadminist011
All Posts
How Teledentistry Is Removing Barriers to Dental Care
Until the pandemic, people never realized how much they would come to rely on virtual solutions. Digital communications have changed the way people communicate, shop, engage socially, and even manage…
bbadminist011
All Posts
April Is Here: That Means Flowers and National Facial Protection Month
Cities and states across the country have gradually lifted mask mandates that were imposed during the outbreak of COVID-19 and its variants. Generally speaking, no states are now directing people…
bbadminist011
All Posts
Looking for the Best Electric Toothbrush? Here Are Some Tips to Guide Your Decision
According to data from the Oral Health Foundation, 12 million Brits have switched to electric toothbrushes over the last five years. An estimated 34 million U.K. adults, 67% of the…
bbadminist011
All Posts
With Expanded Vaccinations and Safety Practices, There’s No Reason to Skip the Dentist
Prior to the pandemic, a disconcerting number of U.S. adults had routinely skipped visits to the dentist for basic care. Since the outbreak of COVID-19, those numbers have risen dramatically.…
Blende Dental Group
All Posts
COVID-19: What a Headache, What a Toothache
It’s probably not shocking news to most people that a resurgence of COVID-19 has come roaring back during the holiday season. Health officials warned early in the summer months that…
Blende Dental Group
All Posts
Preventative Care Is Essential to the Nation’s Homebound as COVID-19 Surges
The recent surge in coronavirus cases hasn’t just led to an alarming rise in hospitalizations and illness, it’s also forced officials in New York and California to reinstate shelter-in-place orders…
Blende Dental Group
All Posts
House call dental care for a homebound society
San Francisco/New York, May 6, 2020 — House Call Dentists announces the expansion and enhancement of its innovative dental care model to safely accommodate emergencies during this time of crisis.…
Blende Dental Group
All Posts
Activated Charcoal on Teeth – Is it Safe?
Activated charcoal is everywhere — from supplement pills to pressed juices to face masks. But is it safe to use on your teeth? Proponents say that brushing with activated charcoal…
Blende Dental Group
All Posts
What You Need to Know About Gum Care
There is no magic when it comes to maintaining the health of your gums. The key to a healthy smile is to make sure you are effectively removing the soft…
Blende Dental Group
All Posts
Patient Safety – What sets us apart?
The Blende Group and House Call Dentists have a unique expertise and service offering, which requires a unique set of skills. But we know skills and safety go hand in…
Blende Dental Group
All Posts
Dental Care Tips for Dementia Caregivers
BY ALZHEIMER'S ASSOCIATION Dental care is one of the most challenging aspects of Alzheimer’s and dementia caregiving. Proper oral care is necessary to prevent eating difficulties, digestive problems and infections.…
Blende Dental Group
All Posts
Xerostomia – The villain known as DRY MOUTH
by Blende Dental Group Seniors often suffer from Dry Mouth, which is a lack of sufficient saliva, making your mouth feel like a desert. However, Dry Mouth is not a…
Blende Dental Group
All Posts
Raising the bar: our standards for being a House Call Dentist
House call dentistry is a unique and highly specialized field. This requires providers that are properly vetted to take care of the vulnerable population they serve. In today’s blog we…
Blende Dental Group
All Posts
Resolutions Revisited – Diet trends and dental health
Happy New Year from the Blende Dental Group! 2017 is a new year, bringing with it a new opportunity to recommit to resolutions of health, like weight loss or adopting…
Blende Dental Group
All Posts
Recreational Cannabis and Oral Health
“Researchers have found that frequent recreational cannabis use – including marijuana, hashish, and hash oil – may be associated with elevated risk of periodontal (gum) disease.” The study recently published…
Blende Dental Group
All Posts
Sarah Marie
Sarah Marie is 90 years old and has dementia. Age Song’s memory care unit in San Francisco referred her to the practice. By performing a simple house call to her…
bbadminist011
All Posts
Fears and Phobias
Have you ever postponed or canceled a dental appointment because the thought of sitting in the dentist’s chair made you feel uncomfortable, nervous, or afraid? While sitting in the waiting…
bbadminist011
All Posts
Drug addiction & oral health
The Blende Dental Group focuses on treating patients with special needs, including those with chemical, or behavioral addictions. If you would like schedule an appointment or speak with a Patient…
bbadminist011
All Posts
Emergency Services FAQ
We offer the following emergency treatments: • Diagnosis & Treatment • Crowns, Bridges, Veneers • Extractions • Infections / Abscesses • Denture Adjustments • Root Canals • Pain Management Contact…
bbadminist011
All Posts
Patients with Head and Neck Cancer Need Comprehensive Dental Treatment
The Blende Dental Group focuses on treating patients with special needs, including those with head and neck cancer. Patients with head and neck cancer are often diagnosed in the later…
bbadminist011
Dental Health
This July 4, Let’s Focus on the Oral Health of Seniors Who Struggle with Independence
With the July 4 holiday right around the corner, the nation gathers to reflect on the nature of independence. Through fraught and bold decisions, the would-be founders of the United…
bbadminist011
Dental Emergencies
How to Know if You’re Having a Dental Emergency
It can be difficult to know when a dental problem is a true emergency and when it can wait for a regular appointment. A severe toothache or a knocked-out tooth…
bbadminist011
Oral Hygiene
Oral Health Care for Seniors: Maintaining Pearly Whites in the Golden Years
As we age, oral health becomes increasingly important for maintaining overall wellbeing. Seniors often face unique challenges when it comes to dental care, from natural aging processes to specific health…
bbadminist011
All Posts
June Is Oral Health Month: Time for a Shiny Summer Smile
Oral Health Month is a reminder of how dental hygiene contributes to our overall health and well-being. As the Mayo Clinic points out, the mouth can be a window to…
bbadminist011
Dental Health
Ozempic Teeth: Protecting Your Oral Health While on GLP-1 Agonists
In recent years, medications like Ozempic, Wegovy, and other GLP-1 receptor agonists have revolutionized diabetes management and weight loss. Millions have experienced significant health benefits from these drugs, ranging from…
bbadminist011
News
One College Senior’s Journey of Hope for People with Disabilities
Ole Miss senior Cameron Geranios may be completing his undergraduate education, but his commitment to the North Mississippi community he’s embraced and his philanthropic endeavors with the Pi Kappa Phi…
bbadminist011
Dental Health
Inflammation Caused by Diets Could Be Fueling Gum Disease and Systemic Illness
Foods that produce inflammation can lead to a host of other chronic problems. Recent research has revealed a concerning link between the health of our mouths and the food we…
bbadminist011
Dental House Calls
For Homebound Seniors, Consider the Gift of Oral Health for Mother’s Day
With Mother’s Day fast approaching, people around the country are preparing to pay tribute to the matriarchs of their families. Celebrations often include outings, gifts, flowers, cards, and meals at…
bbadminist011
Sedation Dentistry
Sedation Dentistry for Seniors: Gentle Care for Golden Years
Sedation dentistry for seniors is a compassionate and effective solution for the barriers that can arise during the aging process. Maintaining good health is a lifelong journey, and oral health…
bbadminist011
Sedation Dentistry
Sedation Dentistry for Special Needs Patients
Sedation dentistry for special needs patients is not just a convenience but often a necessity. Traditional dentistry focuses on reactive care—addressing problems as they arise—with a “one size fits all”…
bbadminist011
Sedation Dentistry
Conquer Dental Anxiety with Sedation Dentistry: Don’t Let Fear Destroy Your Smile
Millions of people experience dental anxiety or its more severe form, dental phobia. It’s a real, often overwhelming feeling, but it doesn't have to control your oral health or your…
bbadminist011
Dental Emergencies
Dental Emergencies: What to Do in a Dental Crisis
Dental emergencies can strike at any moment, often when you least expect them. A sudden and sharp toothache, a knocked-out tooth, or a severe gum infection can disrupt your life…
bbadminist011
Cancer
Oral Cancer Awareness Month: Time for a Spring Screening
More than 65% of working adults put off essential visits to the dentist. Their reasons vary. Some cite rigorous work schedules or family commitments that absorb much of their free…
bbadminist011
Dental Health
Value-Based Oral Health Care: Aligning with WHO’s Global Strategy on Oral Health
Oral health is an essential component of overall health and well-being. Value-based oral health care is the bridge between the mouth and the body. However, traditional dental care has often…
bbadminist011
Dental Health
World Oral Health Day 2025: How Oral Health Improves Mental Health
World Oral Health Day 2025, which falls on March 20, is a global initiative aimed at raising awareness about the critical importance of oral health and its profound impact on…
bbadminist011
Sedation Dentistry
Alzheimer’s Disease and Dentistry: Navigating Oral Health Challenges
Alzheimer’s disease is a progressive neurodegenerative disorder that primarily affects memory, cognitive function, and behavior. As the disease advances, patients face increasing challenges in managing their daily routines. That includes…
bbadminist011
Sedation Dentistry
Sedation Dentistry: A Safe and Stress-Free Approach to Dental Care
Sedation dentistry represents a breakthrough in dental care for patients. Dental anxiety and fear are common barriers that prevent many individuals from seeking the dental care they need. At Blende…
bbadminist011
Dental Health
The Oral Microbiome: How the Mouth Affects the Body and Why Value-Based Dentistry Is Key to Overall Health
There is an intricate relationship between oral and overall health. What goes on in your mouth can manifest into what happens in the rest of your body. The oral microbiome—a…
bbadminist011
Dental Health
Valentine’s Day and Your Oral Health: a Smile Worth Falling For
Valentine’s Day is all about love, romance, and probably a kiss or two. It’s a holiday when sweethearts and sweet treats come together. So this makes Valentine’s a great day…
bbadminist011
Dental Safety
Is Sedation Dentistry Safe? Yes, with the Right Dentist. Here’s What to Know
Sedation dentistry can elevate the patient experience and deliver predictable outcomes, especially for people with anxiety or dental fear (dentophobia), disabilities, and cognitive impairments. Modern dental techniques have transformed the…
bbadminist011
Dental Health
Climate Change Is Fueling Wildfires and Disasters; Sustainable Dentistry Can Make a Difference
The deadly California wildfires provide another stark reminder that the effects of climate change will continue to increase the prevalence of natural disasters across the country. The California Air Resources…
bbadminist011
Dental Innovations
Dental Trends of 2025: Insights for General, Special Needs, and In-Home Dentistry
Looking at the dental trends shaping the industry in 2025, it’s important to understand the unprecedented pace at which dentistry is evolving. Advancements in technology, changes in patient demographics, and…
bbadminist011
All Posts
Celebrating a Season of Smiles: Happy Holidays from the Blende Dental Group
Happy holidays! As the winter holidays approach and 2024 draws to a close, we at the Blende Dental Group make sure to take time out from our routines to reflect…
bbadminist011
All Posts
Gratitude in Every Smile: A Thanksgiving Message from the Blende Dental Group
As the autumn leaves blanket the ground and the aroma of Thanksgiving feasts fills the air, we find ourselves reflecting on the many blessings that have graced our lives. This…
bbadminist011
Special Needs
Overcoming the Barriers to Accessible Dental Care for Disabled People
Disabled people, through their resilience and fortitude, have demonstrated throughout history their strength in overcoming obstacles. However, those challenges are more difficult to conquer when the barriers they face are…
bbadminist011
Dental Safety
The Dangers of Unlicensed Dentists: What You Need to Know
Lately, alarming news reports have highlighted the growing issue of unlicensed dentists operating in various communities. These illegal practitioners pose significant risks to public health and safety. As a reputable…
bbadminist011
Special Needs
Autism Acceptance Month: The Importance of Oral Health Care for People with ASD
In recognition of Autism Acceptance Month, the Blende Dental Group is emphasizing the importance of oral health care for individuals with Autism Spectrum Disorder (ASD). They face unique challenges when…
bbadminist011
Dental Innovations
Nanotechnology Could Revolutionize Dentistry: Tiny Tech for Big Smiles
Nanotechnology deals with the manipulation of materials at the atomic and molecular level, leading to the creation of particles with unique properties. Like robots, sentient computers, and bionic implants, it’s…
bbadminist011
Dental Health
Hay Fever and Your Smile: The Link Between Allergies and Oral Health
Spring is in the air, and so too are the pollens that lead to hay fever. If you suffer from seasonal allergies, you’re well-acquainted with itchy eyes, sneezing fits, and…
bbadminist011
Cancer
Colorectal Cancer Risk and Oral Health: the Mouth-Body Connection
Colorectal cancer is the second most common cause of cancer deaths, according to the American Cancer Society. And your oral health could play an important role in preventing it. Unlike…
bbadminist011
Oral Hygiene
Easter Smiles: Sweet Treats and Healthy Teeth
Easter began as an ancient pagan rite, but in the 1700s, the holiday transformed and introduced a new mascot. Since then, the Easter Bunny has been delivering treats to children…
bbadminist011
Dental Health
Menopause and Oral Health: The Link Between Hormonal Shifts and a Healthy Smile
For many women, menopause marks a significant shift in their physical and emotional wellbeing. Hot flashes, night sweats, and mood swings are often the first symptoms that come to mind.…
bbadminist011
Oral Hygiene
Exploring Natural Oral Hygiene Products
Consumers today are increasingly interested in natural and holistic approaches to wellness, and oral hygiene is no exception. This shift reflects a desire to understand what we put in and…
bbadminist011
Dental Health
Oral Health Literacy: Empowering Optimal Dental Outcomes
Oral health literacy is a growing area of focus in dentistry, and we at the Blende Dental Group are dedicated to empowering our patients with the knowledge they need to…
bbadminist011
Dental Health
Understanding and Strengthening Weak Tooth Enamel for a Confident Smile
Tooth enamel is the armor that helps protect our teeth. However, not all enamel is created equally. Strong, healthy teeth are the foundation of a confident smile. They not only…
bbadminist011
Dental Health
New Bad Breath Research Unravels the Secrets of Halitosis and Potential Treatments
Bad breath, also known as halitosis, can be an embarrassing and socially isolating issue. However, the key to fresher breath may not simply be achieved by brushing and flossing more;…
bbadminist011
Oral Hygiene
Dental Care Tips for a Sparkling Valentine’s Day
Valentine’s Day is all about hearts, flowers, and smiles – and a healthy smile plays a crucial role in expressing love and confidence. Beyond the aesthetics, proper oral care contributes…
bbadminist011
Special Needs
Smiles for All: Celebrating Children’s Dental Health Month with Special Needs in Mind
February is National Children's Dental Health Month, a time to focus on the importance of oral health for our little ones. However, for parents and caregivers of children with special…
bbadminist011
Dental Innovations
The Rise of Minimally Invasive Dentistry
The shift toward minimally invasive dentistry is gaining momentum as advanced technology becomes more of a mainstay in modern dentistry. This transformative approach focuses on reducing the use of traditional…
bbadminist011
Dental Innovations
Seeing Beyond the Surface: Advanced Dental Imaging and AI May Revolutionize Oral Health
Advanced dental imaging technologies aren’t just about taking better pictures, they represent a new way to unlock deeper levels of understanding and precision in oral health care. The grainy and…
bbadminist011
Uncategorized
Dental Trends of 2024: New Tech, Personalized Care, and Overall Health
Contrary to what people may believe, the dental industry is not a static and analog institution. The dental trends of 2024 demonstrate the dynamism of the practice and its rapid…
bbadminist011
Oral Hygiene
Don’t Let Bad Breath Sour Your Wonderful Holiday Experiences
Halitosis, otherwise known as bad breath, can keep you at a distance from those you long to be near. And you can have it without realizing it. From the plethora…
bbadminist011
Dental Innovations
The Evolving Landscape of Modern Dentistry: Stem Cells, Technology, Pain Management, and Future Trends
In recent years, modern dentistry has witnessed a wave of transformative developments that are reshaping the way we approach oral health. From harnessing the regenerative potential of stem cells to…
bbadminist011
All Posts
Understanding TMJ Disorders: Shedding Light During TMJ Awareness Month
TMJ disorders are prevalent but not always fully comprehended. November is TMJ Awareness Month, a time when we come together to learn about this often misunderstood condition, its symptoms, causes,…
bbadminist011
All Posts
National Brush Day Celebrates the Toothbrush. But Just How Did the Most Famous Dental Device Come to Be?
With Halloween behind us and more holidays on the way, along with a bevy of sweets and treats, it’s no coincidence that National Brush Day is observed on November 1…
bbadminist011
Dental Health
Don’t Let Halloween Treats Become Oral Health Horror Stories
The bewitching season is upon us, and Halloween is lurking around the corner with its spooky charms and delightful confections. It’s a time when kids and adults revel in dressing…
bbadminist011
Dental Health
It’s National Seafood Month, Time to Explore the Oral Health Benefits of Seafood for Those Pearly Whites
This National Seafood Month, explore the incredible oral health benefits of seafood and how it can transform your smile. October is National Seafood Month, a time to celebrate the bountiful…
bbadminist011
Dental Health
Mental Health Issues Affect Oral Health, But Specialized Dental Care Is Available
Each year, millions of Americans face the reality of living with mental health issues, but because of persistent stigmas and the fear of discussing these conditions, too few people seek…
bbadminist011
Dental Health
The Future of Dentistry: Embracing Innovation and Personalization
The future of dentistry is defined by innovation in techniques and technologies, with an emphasis on personalization and comfort. For those concerned about their oral health, a brighter future and…
bbadminist011
Oral Hygiene
October Is National Dental Hygiene Month – Tips and Tricks for Treating Yourself to a Cleaner Mouth
In 2009, the American Dental Hygienists’ Association (ADHA) helped launch National Dental Hygiene Month, which has been recognized annually in October since its inception. ADHA took these steps because it…
bbadminist011
All Posts
No White After Labor Day Shouldn’t Apply to Your Teeth: Here Are Some Tips for a Stunning Smile All Year
Outdated though the traditional may be, you could still face criticism from fashionistas for wearing white after Labor Day, a faux pas that invokes a throwback to the turn of…
bbadminist011
News
Happy Holidays from the Blende Dental Group
The end of any year is always a time of reflection. And when we look back on 2022, despite the challenges it presented around the world, we can't help but…
bbadminist011
Dental Health
How Dentistry Has Changed to Support Patients in the New Normal of Digital, On Demand, Concierge Care
According to research from the Federal Reserve Bank of New York, Americans got back 60 million hours of their time as a result of remote work during the pandemic. So…
bbadminist011
All Posts
Happy Thanksgiving from the Blende Dental Group
Thanksgiving is tomorrow, and as we write this, families across the nation are preparing to gather in a celebration of the bonds that unite us. The spirit of this season…
bbadminist011
All Posts
You May Be Surprised to Learn that Dental House Calls Not Only Exist, They’re Thriving
House calls are firmly ingrained in the fabric of American culture and history. We’ve all heard stories about the country doctor who traveled across hill and dale to care for…
bbadminist011
All Posts
No Tricks, Just Tips for a Healthy Mouth this Halloween
With Halloween falling on a Monday this year, weekend gatherings and All Hallows Eve trick-or-treating mean costumed revelers may have three days’ worth of sweets and goodies to enjoy. That’s…
bbadminist011
All Posts
Virtual Reality Could Become a Real World Benefit to Dentists and Their Patients
With leaps in the development of Virtual Reality (VR), could dentistry become part of Mark Zuckerberg’s metaverse? VR is being used as an educational tool for students and as an…
bbadminist011
All Posts
Blende Dental Group Thrilled to Participate in the International Association for Disability and Oral Health Conference in Paris
From August 23 to 26, the 26th conference of the International Association for Disability and Oral Health (iADH) takes place in Paris. “The rights of vulnerable populations to achieve an…
bbadminist011
All Posts
Cigarettes, Vapes and Marijuana, Oh My: The Oral Health Risks of Smoking
The good news? Tobacco use has reached an historic low. The bad news? Vaping (using electronic cigarettes filled with juice or nicotine salt) and marijuana use are climbing. Vaping may…
bbadminist011
All Posts
The Cosmetic Dentistry Market Is Booming, Thanks to Technology and Technique
According to the July report “Cosmetic Dentistry Market Size, Share, Trends, By Product Type, By Patient Type, By End-Use, and By Region Forecast to 2028,” cosmetic dentistry is booming. Analysts…
bbadminist011
All Posts
People with Special Needs Are Facing a Growing But Seldom Discussed Oral Health Crisis
It requires little effort to peruse the daily news and uncover stories related to the growing health crisis in the country, whether the issues involve post-pandemic outbreaks, staffing shortages for…
bbadminist011
All Posts
How Artificial Intelligence Will Shape the Future Reality of Dentistry
Artificial Intelligence (AI) and Augmented Intelligence (AuI), once inhabitants of a realm relegated to science fiction, have become increasingly ubiquitous aspects of modern life. Every day, people tap into the…
bbadminist011
All Posts
Bad Brushing Habits: Elbow Grease and Antiseptic Mouthwash Aren’t the Answer to Healthy Teeth
There’s an old joke that goes, “You brush your teeth at night to keep your teeth, you brush your teeth in the morning to keep your friends.” Humor aside, the…
bbadminist011
All Posts
Proudly Display a Healthier Smile this LGBTQ+ Pride Month
June 1 marks the first day of LGBTQ+ Pride Month. Equality, inclusion, acceptance, and support for friends and loved ones in the community are critical to the advancement of our…
bbadminist011
All Posts
Over-the-Counter or Professional Teeth Whitening? For the Brightest Smile, See Your Dentist
Memorial Day is right around the corner, signaling the start of summer. It’s also the season when people return to wearing white. However, the quest for a brighter, whiter smile…
bbadminist011
All Posts
You May Be Surprised at How Your Dentist Can Help with Sleep Apnea
May is a month of many health awareness events, including sleep. Created by the Better Sleep Council (BSC), Better Sleep Month seeks to raise awareness about the benefits associated with…
bbadminist011
All Posts
Before Ordering Another Round, Know How Alcohol Affects Oral Health
Need a drink after a rough day? Is it “beer-thirty” yet? Are you meeting colleagues for an adult beverage at the local happy hour? Have you been to Napa and…
bbadminist011
All Posts
Asthma, Allergies, and Dental Problems: What You Need to Know
In 1984, the Asthma and Allergy Foundation of America (AAFA) declared the month of May to be “National Asthma and Allergy Awareness Month.” They chose this time of year because…
bbadminist011
All Posts
Yes, Kissing Can Cause Cavities, So Plan a Date with Your Dentist Before Your Tinder Match
All the kids are on TikTok, they say. TikTok has emerged as an immensely popular social network that relies on short-form user videos that span genres such as pranks, stunts,…
bbadminist011
All Posts
Braces or Clear Aligners? The Choice Involves More than Appearance
For many teens and adults, orthodontics offers a clear path toward straighter teeth and a more confident smile. Misaligned teeth are common and don’t generally pose oral health risks. So…
bbadminist011
All Posts
Everyone’s Stressed Out, and It’s a Real Pain in the…Mouth
We learned a lot during the past two years of dealing with a pandemic. For many people, one of those things was the word “bruxism.” Dentists around the country have…
bbadminist011
All Posts
It’s Time to See the Dentist and Overcome the Pandemic’s “Dental Disaster”
Health officials are warning of fresh COVID-19 outbreaks with new variants such as BA.2.12 and BA.2.12.1, surging across the United States. The fallout from the pandemic’s initial outbreak severely impacted…
bbadminist011
All Posts
How Teledentistry Is Removing Barriers to Dental Care
Until the pandemic, people never realized how much they would come to rely on virtual solutions. Digital communications have changed the way people communicate, shop, engage socially, and even manage…
bbadminist011
All Posts
April Is Here: That Means Flowers and National Facial Protection Month
Cities and states across the country have gradually lifted mask mandates that were imposed during the outbreak of COVID-19 and its variants. Generally speaking, no states are now directing people…
bbadminist011
All Posts
Looking for the Best Electric Toothbrush? Here Are Some Tips to Guide Your Decision
According to data from the Oral Health Foundation, 12 million Brits have switched to electric toothbrushes over the last five years. An estimated 34 million U.K. adults, 67% of the…
bbadminist011
All Posts
With Expanded Vaccinations and Safety Practices, There’s No Reason to Skip the Dentist
Prior to the pandemic, a disconcerting number of U.S. adults had routinely skipped visits to the dentist for basic care. Since the outbreak of COVID-19, those numbers have risen dramatically.…
Blende Dental Group
All Posts
COVID-19: What a Headache, What a Toothache
It’s probably not shocking news to most people that a resurgence of COVID-19 has come roaring back during the holiday season. Health officials warned early in the summer months that…
Blende Dental Group
All Posts
Preventative Care Is Essential to the Nation’s Homebound as COVID-19 Surges
The recent surge in coronavirus cases hasn’t just led to an alarming rise in hospitalizations and illness, it’s also forced officials in New York and California to reinstate shelter-in-place orders…
Blende Dental Group
All Posts
House call dental care for a homebound society
San Francisco/New York, May 6, 2020 — House Call Dentists announces the expansion and enhancement of its innovative dental care model to safely accommodate emergencies during this time of crisis.…
Blende Dental Group
All Posts
Activated Charcoal on Teeth – Is it Safe?
Activated charcoal is everywhere — from supplement pills to pressed juices to face masks. But is it safe to use on your teeth? Proponents say that brushing with activated charcoal…
Blende Dental Group
All Posts
What You Need to Know About Gum Care
There is no magic when it comes to maintaining the health of your gums. The key to a healthy smile is to make sure you are effectively removing the soft…
Blende Dental Group
All Posts
Patient Safety – What sets us apart?
The Blende Group and House Call Dentists have a unique expertise and service offering, which requires a unique set of skills. But we know skills and safety go hand in…
Blende Dental Group
All Posts
Dental Care Tips for Dementia Caregivers
BY ALZHEIMER'S ASSOCIATION Dental care is one of the most challenging aspects of Alzheimer’s and dementia caregiving. Proper oral care is necessary to prevent eating difficulties, digestive problems and infections.…
Blende Dental Group
All Posts
Xerostomia – The villain known as DRY MOUTH
by Blende Dental Group Seniors often suffer from Dry Mouth, which is a lack of sufficient saliva, making your mouth feel like a desert. However, Dry Mouth is not a…
Blende Dental Group
All Posts
Raising the bar: our standards for being a House Call Dentist
House call dentistry is a unique and highly specialized field. This requires providers that are properly vetted to take care of the vulnerable population they serve. In today’s blog we…
Blende Dental Group
All Posts
Resolutions Revisited – Diet trends and dental health
Happy New Year from the Blende Dental Group! 2017 is a new year, bringing with it a new opportunity to recommit to resolutions of health, like weight loss or adopting…
Blende Dental Group
All Posts
Recreational Cannabis and Oral Health
“Researchers have found that frequent recreational cannabis use – including marijuana, hashish, and hash oil – may be associated with elevated risk of periodontal (gum) disease.” The study recently published…
Blende Dental Group
All Posts
Sarah Marie
Sarah Marie is 90 years old and has dementia. Age Song’s memory care unit in San Francisco referred her to the practice. By performing a simple house call to her…
bbadminist011
All Posts
Fears and Phobias
Have you ever postponed or canceled a dental appointment because the thought of sitting in the dentist’s chair made you feel uncomfortable, nervous, or afraid? While sitting in the waiting…
bbadminist011
All Posts
Drug addiction & oral health
The Blende Dental Group focuses on treating patients with special needs, including those with chemical, or behavioral addictions. If you would like schedule an appointment or speak with a Patient…
bbadminist011
All Posts
Emergency Services FAQ
We offer the following emergency treatments: • Diagnosis & Treatment • Crowns, Bridges, Veneers • Extractions • Infections / Abscesses • Denture Adjustments • Root Canals • Pain Management Contact…
bbadminist011
All Posts
Patients with Head and Neck Cancer Need Comprehensive Dental Treatment
The Blende Dental Group focuses on treating patients with special needs, including those with head and neck cancer. Patients with head and neck cancer are often diagnosed in the later…
bbadminist011
Dental Health
This July 4, Let’s Focus on the Oral Health of Seniors Who Struggle with Independence
With the July 4 holiday right around the corner, the nation gathers to reflect on the nature of independence. Through fraught and bold decisions, the would-be founders of the United…
bbadminist011
Dental Emergencies
How to Know if You’re Having a Dental Emergency
It can be difficult to know when a dental problem is a true emergency and when it can wait for a regular appointment. A severe toothache or a knocked-out tooth…
bbadminist011
Oral Hygiene
Oral Health Care for Seniors: Maintaining Pearly Whites in the Golden Years
As we age, oral health becomes increasingly important for maintaining overall wellbeing. Seniors often face unique challenges when it comes to dental care, from natural aging processes to specific health…
bbadminist011
All Posts
June Is Oral Health Month: Time for a Shiny Summer Smile
Oral Health Month is a reminder of how dental hygiene contributes to our overall health and well-being. As the Mayo Clinic points out, the mouth can be a window to…
bbadminist011
Dental Health
Ozempic Teeth: Protecting Your Oral Health While on GLP-1 Agonists
In recent years, medications like Ozempic, Wegovy, and other GLP-1 receptor agonists have revolutionized diabetes management and weight loss. Millions have experienced significant health benefits from these drugs, ranging from…
bbadminist011
News
One College Senior’s Journey of Hope for People with Disabilities
Ole Miss senior Cameron Geranios may be completing his undergraduate education, but his commitment to the North Mississippi community he’s embraced and his philanthropic endeavors with the Pi Kappa Phi…
bbadminist011
Dental Health
Inflammation Caused by Diets Could Be Fueling Gum Disease and Systemic Illness
Foods that produce inflammation can lead to a host of other chronic problems. Recent research has revealed a concerning link between the health of our mouths and the food we…
bbadminist011
Dental House Calls
For Homebound Seniors, Consider the Gift of Oral Health for Mother’s Day
With Mother’s Day fast approaching, people around the country are preparing to pay tribute to the matriarchs of their families. Celebrations often include outings, gifts, flowers, cards, and meals at…
bbadminist011
Sedation Dentistry
Sedation Dentistry for Seniors: Gentle Care for Golden Years
Sedation dentistry for seniors is a compassionate and effective solution for the barriers that can arise during the aging process. Maintaining good health is a lifelong journey, and oral health…
bbadminist011
Sedation Dentistry
Sedation Dentistry for Special Needs Patients
Sedation dentistry for special needs patients is not just a convenience but often a necessity. Traditional dentistry focuses on reactive care—addressing problems as they arise—with a “one size fits all”…
bbadminist011
Sedation Dentistry
Conquer Dental Anxiety with Sedation Dentistry: Don’t Let Fear Destroy Your Smile
Millions of people experience dental anxiety or its more severe form, dental phobia. It’s a real, often overwhelming feeling, but it doesn't have to control your oral health or your…
bbadminist011
Dental Emergencies
Dental Emergencies: What to Do in a Dental Crisis
Dental emergencies can strike at any moment, often when you least expect them. A sudden and sharp toothache, a knocked-out tooth, or a severe gum infection can disrupt your life…
bbadminist011
Cancer
Oral Cancer Awareness Month: Time for a Spring Screening
More than 65% of working adults put off essential visits to the dentist. Their reasons vary. Some cite rigorous work schedules or family commitments that absorb much of their free…
bbadminist011
Dental Health
Value-Based Oral Health Care: Aligning with WHO’s Global Strategy on Oral Health
Oral health is an essential component of overall health and well-being. Value-based oral health care is the bridge between the mouth and the body. However, traditional dental care has often…
bbadminist011
Dental Health
World Oral Health Day 2025: How Oral Health Improves Mental Health
World Oral Health Day 2025, which falls on March 20, is a global initiative aimed at raising awareness about the critical importance of oral health and its profound impact on…
bbadminist011
Sedation Dentistry
Alzheimer’s Disease and Dentistry: Navigating Oral Health Challenges
Alzheimer’s disease is a progressive neurodegenerative disorder that primarily affects memory, cognitive function, and behavior. As the disease advances, patients face increasing challenges in managing their daily routines. That includes…
bbadminist011
Sedation Dentistry
Sedation Dentistry: A Safe and Stress-Free Approach to Dental Care
Sedation dentistry represents a breakthrough in dental care for patients. Dental anxiety and fear are common barriers that prevent many individuals from seeking the dental care they need. At Blende…
bbadminist011
Dental Health
The Oral Microbiome: How the Mouth Affects the Body and Why Value-Based Dentistry Is Key to Overall Health
There is an intricate relationship between oral and overall health. What goes on in your mouth can manifest into what happens in the rest of your body. The oral microbiome—a…
bbadminist011
Dental Health
Valentine’s Day and Your Oral Health: a Smile Worth Falling For
Valentine’s Day is all about love, romance, and probably a kiss or two. It’s a holiday when sweethearts and sweet treats come together. So this makes Valentine’s a great day…
bbadminist011
Dental Safety
Is Sedation Dentistry Safe? Yes, with the Right Dentist. Here’s What to Know
Sedation dentistry can elevate the patient experience and deliver predictable outcomes, especially for people with anxiety or dental fear (dentophobia), disabilities, and cognitive impairments. Modern dental techniques have transformed the…
bbadminist011
Dental Health
Climate Change Is Fueling Wildfires and Disasters; Sustainable Dentistry Can Make a Difference
The deadly California wildfires provide another stark reminder that the effects of climate change will continue to increase the prevalence of natural disasters across the country. The California Air Resources…
bbadminist011
Dental Innovations
Dental Trends of 2025: Insights for General, Special Needs, and In-Home Dentistry
Looking at the dental trends shaping the industry in 2025, it’s important to understand the unprecedented pace at which dentistry is evolving. Advancements in technology, changes in patient demographics, and…
bbadminist011
All Posts
Celebrating a Season of Smiles: Happy Holidays from the Blende Dental Group
Happy holidays! As the winter holidays approach and 2024 draws to a close, we at the Blende Dental Group make sure to take time out from our routines to reflect…
bbadminist011
All Posts
Gratitude in Every Smile: A Thanksgiving Message from the Blende Dental Group
As the autumn leaves blanket the ground and the aroma of Thanksgiving feasts fills the air, we find ourselves reflecting on the many blessings that have graced our lives. This…
bbadminist011
Special Needs
Overcoming the Barriers to Accessible Dental Care for Disabled People
Disabled people, through their resilience and fortitude, have demonstrated throughout history their strength in overcoming obstacles. However, those challenges are more difficult to conquer when the barriers they face are…
bbadminist011
Dental Safety
The Dangers of Unlicensed Dentists: What You Need to Know
Lately, alarming news reports have highlighted the growing issue of unlicensed dentists operating in various communities. These illegal practitioners pose significant risks to public health and safety. As a reputable…
bbadminist011
Special Needs
Autism Acceptance Month: The Importance of Oral Health Care for People with ASD
In recognition of Autism Acceptance Month, the Blende Dental Group is emphasizing the importance of oral health care for individuals with Autism Spectrum Disorder (ASD). They face unique challenges when…
bbadminist011
Dental Innovations
Nanotechnology Could Revolutionize Dentistry: Tiny Tech for Big Smiles
Nanotechnology deals with the manipulation of materials at the atomic and molecular level, leading to the creation of particles with unique properties. Like robots, sentient computers, and bionic implants, it’s…
bbadminist011
Dental Health
Hay Fever and Your Smile: The Link Between Allergies and Oral Health
Spring is in the air, and so too are the pollens that lead to hay fever. If you suffer from seasonal allergies, you’re well-acquainted with itchy eyes, sneezing fits, and…
bbadminist011
Cancer
Colorectal Cancer Risk and Oral Health: the Mouth-Body Connection
Colorectal cancer is the second most common cause of cancer deaths, according to the American Cancer Society. And your oral health could play an important role in preventing it. Unlike…
bbadminist011
Oral Hygiene
Easter Smiles: Sweet Treats and Healthy Teeth
Easter began as an ancient pagan rite, but in the 1700s, the holiday transformed and introduced a new mascot. Since then, the Easter Bunny has been delivering treats to children…
bbadminist011
Dental Health
Menopause and Oral Health: The Link Between Hormonal Shifts and a Healthy Smile
For many women, menopause marks a significant shift in their physical and emotional wellbeing. Hot flashes, night sweats, and mood swings are often the first symptoms that come to mind.…
bbadminist011
Oral Hygiene
Exploring Natural Oral Hygiene Products
Consumers today are increasingly interested in natural and holistic approaches to wellness, and oral hygiene is no exception. This shift reflects a desire to understand what we put in and…
bbadminist011
Dental Health
Oral Health Literacy: Empowering Optimal Dental Outcomes
Oral health literacy is a growing area of focus in dentistry, and we at the Blende Dental Group are dedicated to empowering our patients with the knowledge they need to…
bbadminist011
Dental Health
Understanding and Strengthening Weak Tooth Enamel for a Confident Smile
Tooth enamel is the armor that helps protect our teeth. However, not all enamel is created equally. Strong, healthy teeth are the foundation of a confident smile. They not only…
bbadminist011
Dental Health
New Bad Breath Research Unravels the Secrets of Halitosis and Potential Treatments
Bad breath, also known as halitosis, can be an embarrassing and socially isolating issue. However, the key to fresher breath may not simply be achieved by brushing and flossing more;…
bbadminist011
Oral Hygiene
Dental Care Tips for a Sparkling Valentine’s Day
Valentine’s Day is all about hearts, flowers, and smiles – and a healthy smile plays a crucial role in expressing love and confidence. Beyond the aesthetics, proper oral care contributes…
bbadminist011
Special Needs
Smiles for All: Celebrating Children’s Dental Health Month with Special Needs in Mind
February is National Children's Dental Health Month, a time to focus on the importance of oral health for our little ones. However, for parents and caregivers of children with special…
bbadminist011
Dental Innovations
The Rise of Minimally Invasive Dentistry
The shift toward minimally invasive dentistry is gaining momentum as advanced technology becomes more of a mainstay in modern dentistry. This transformative approach focuses on reducing the use of traditional…
bbadminist011
Dental Innovations
Seeing Beyond the Surface: Advanced Dental Imaging and AI May Revolutionize Oral Health
Advanced dental imaging technologies aren’t just about taking better pictures, they represent a new way to unlock deeper levels of understanding and precision in oral health care. The grainy and…
bbadminist011
Uncategorized
Dental Trends of 2024: New Tech, Personalized Care, and Overall Health
Contrary to what people may believe, the dental industry is not a static and analog institution. The dental trends of 2024 demonstrate the dynamism of the practice and its rapid…
bbadminist011
Oral Hygiene
Don’t Let Bad Breath Sour Your Wonderful Holiday Experiences
Halitosis, otherwise known as bad breath, can keep you at a distance from those you long to be near. And you can have it without realizing it. From the plethora…
bbadminist011
Dental Innovations
The Evolving Landscape of Modern Dentistry: Stem Cells, Technology, Pain Management, and Future Trends
In recent years, modern dentistry has witnessed a wave of transformative developments that are reshaping the way we approach oral health. From harnessing the regenerative potential of stem cells to…
bbadminist011
All Posts
Understanding TMJ Disorders: Shedding Light During TMJ Awareness Month
TMJ disorders are prevalent but not always fully comprehended. November is TMJ Awareness Month, a time when we come together to learn about this often misunderstood condition, its symptoms, causes,…
bbadminist011
All Posts
National Brush Day Celebrates the Toothbrush. But Just How Did the Most Famous Dental Device Come to Be?
With Halloween behind us and more holidays on the way, along with a bevy of sweets and treats, it’s no coincidence that National Brush Day is observed on November 1…
bbadminist011
Dental Health
Don’t Let Halloween Treats Become Oral Health Horror Stories
The bewitching season is upon us, and Halloween is lurking around the corner with its spooky charms and delightful confections. It’s a time when kids and adults revel in dressing…
bbadminist011